Benefits of Digital Stethoscopes During a Pandemic
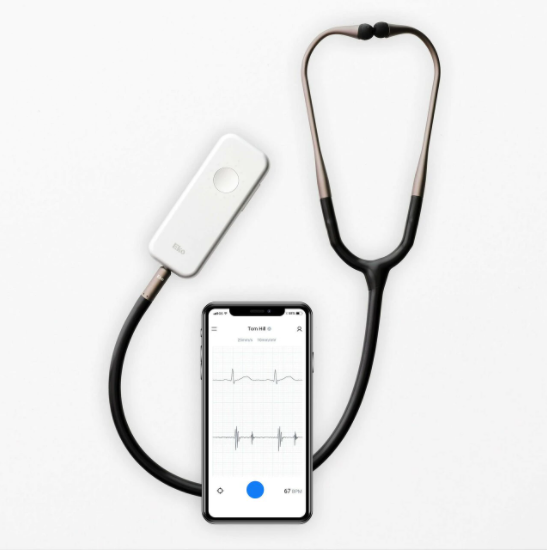
The coronavirus pandemic has forever changed the healthcare landscape and pushed pipeline innovations to the forefront faster than ever. Digital stethoscopes have been around since the 1970s and have been a major disruptor in the fight against heart disease, which is the leading cause of death in almost every country in the world. The COVID era has sent revolutionary healthcare tools such as this to the surface, and digital stethoscopes have served on the frontlines of many global health crises, such as the 2014 Ebola outbreak in Africa. The recent evolution of Ambient Noise Reduction (ANR) and communication technology over the past 10 years have heightened the effectiveness of this much-needed tool yet again.
Digital Stethoscopes Are Much More Than a Fluff Tool
Although revolutionary technological advancements in the medical industry have brought about machines such as the electrocardiogram (ECG), computed tomography (CT), and magnetic resonance imaging (MRI), testing is often expensive, and finding specialists can be difficult. The World Health Organization has reported approximately 80% of cardiovascular-related deaths worldwide are in low to middle-income countries. Thus, electronic stethoscopes have become far more than a nice to have in cases such as this since precise readings can detect anatomical abnormalities in heart valves and heart murmurs that even ECGs may have trouble picking up.
COVID-19 has impeded access to care and added unexpected caveats to patient treatment that the digital stethoscope has helped to overcome. The ability to place the stethoscope on a patient and get a digital reading sent to a mobile device, or loudspeaker outside of a biocontainment unit via Bluetooth, severely slices chances of transmitting deadly diseases. Doctors and care team members no longer have to go in and out of containment units and from patient to patient because of the stethoscope’s wireless capabilities. The likelihood of accuracy is also quite a bit higher, especially if patients are hooked up to other machines or the noise level in the treatment area is high.
Better Accuracy, Better Readings, Better Care
The accuracy component is a significant factor in digitized stethoscopes, and many on the market have a wide range of frequencies that can be used to get the best reading possible. This is usually done through sound amplification that is produced through noise-canceling technology or transducers. There are also settings that suppress other novelty noises (friction, ambient) and a wide array of frequency response modes can be activated to tune into heart and lung sounds, along with sound notes from different parts of the body that can be critical to capture.
The reporting feature is yet another attractive element of this digital tool. Data from the reading can be easily transmitted, collected, stored, and compared for analysis and be sent to a physician, even when taking the reading from home. This feature has boosted healthcare capacity dramatically, and physicians can revisit readings more than once to ensure accuracy, keep an archive, and shift when need be to a different care plan that can save a patient’s life. The ability to access past reporting also makes it possible to collaborate with more specialists regarding care and keep members of a patient’s care team up to date on any changes or abnormalities.
A New Ally in the Age of Telemedicine
At the beginning of the coronavirus pandemic in February 2020, the Centers for Disease Control (CDC) began to widen patient care tunnels and loosened telehealth policies to allow full utilization of a health service that has been emerging since its inception. This change in policy allowed physicians to monitor and interact with patients with cardiovascular issues specifically, and electronic stethoscopes have been a critical part of home healthcare solutions in the age of COVID. Access and insight is an invaluable tool, and routine care became a practice that doesn’t necessarily have to be done in person. Telehealth appointments rose 154% in March 2020, and the U.S. Coronavirus Aid, Relief, and Economic Security (CARES) Act made telehealth services far more cost-effective for patients.
See below for commentary from Dr. Steve Pham, VP of clinical and research affairs at Eko:
- How have these stethoscopes made a difference in your own medical practice?
“In my practice as an emergency medicine physician, I’ve missed abnormal heart sounds when using a traditional stethoscope and not the Eko CORE. I had a young patient – in her twenties, with no history of medical conditions – in for a complaint of chest pain that raised my suspicion for a blood clot in her lungs. I performed a standard rapid auscultation screening, and heard no abnormalities. After a series of tests, to my surprise, I diagnosed her with endocarditis. I immediately reassessed her with a full auscultation exam enhanced by Eko AI and discovered a subtle murmur! If I had been using Eko’s AI functionality in my first exam, my suspicion for endocarditis would have been on the top of my list – as opposed to not even on my radar.
Heart sounds can be extremely difficult to detect – in fact, many clinicians only accurately recognize a small fraction of heart sounds, even after training. But the better clinicians can hear and the better we can screen, the better we can care for our patients.”
- What are the implications of using these stethoscopes/what do they mean for the future of diagnostic testing?
“Eko is working to change how auscultation is done, using cutting-edge machine learning and data science to discover and halt the progression of chronic cardiovascular diseases.
There are clear accessibility advantages that come along with digital stethoscopes. The volume amplification and noise cancellation functionalities are so advanced that clinicians aren’t able to hear ambient noise in the back of an ambulance. Clinicians with hearing difficulties are also able to better hone in on heart and lung sounds – as well as reference in-app sound wave visualizations – to better assess and diagnose conditions.”
- Lastly, how has the pandemic brought this technology to the forefront?
“The outbreak of COVID-19 has caused rapid commoditization and adoption of telehealth. Many companies are looking for opportunities to get involved – by creating video platforms, tools, etc. – but the biggest missing piece in telemedicine is a comprehensive user experience that blends online and offline care delivery.
Telehealth services are only effective if providers get the critical information – and not information overload – they need to accurately assess patient health. With Eko, clinicians are able to virtually examine cardiac and pulmonary health as if they were standing at the bedside.
Recent advancements in telehealth allow expanded access to patient care (particularly to those in rural settings) that can alleviate strain on the health system and reduce unnecessary exposure to COVID-19. As 2021 continues, we can expect to see more progress made within telemedicine to equip physicians with full insight during remote consultation, as well as provide a better, more unified patient experience.”
Below is commentary from Dr. Terry Grossman, founder of Grossman Wellness Center in Denver Colorado:
“The DUO is a game changer. It’s helped me to take care of out of town patients and out of country patients. Having the ability to listen to their heart and listen to their lungs, that’s made a huge difference. And it’s helped patients to realize, hey if I get sick, I can just call my doctor and have him listen to my lungs without traveling halfway around the country or the world.
Typically, the patients who are from out of town would travel to our clinic in Denver to have an annual exam. Over the past six months, it’s been much more difficult for domestic patients. Many of them don’t want to travel by plane, and I don’t blame them. And international patients cannot travel. They don’t have the option. In order to get to the United States, they have to self-quarantine for two weeks and for many of these individuals it’s just not feasible or realistic.
Eko has enabled me to listen to heart, lung and abdominal sounds for annual exams or executive-type physicals. It’s really a hands-on physical that I can perform on a virtual platform. It turns out that the augmented sound available through the Eko stethoscope is better than my high-end cardiology stethoscope that I use in the office. I was able to hear a murmur that I’d never heard before. Then I looked at the Eko software and it said on there, ‘murmur.’ It confirmed what I thought I heard. The AI is quite good.
It really has increased the sense of being cared for. The patients feel I can really listen to them, not just physically, but their story. It’s made an enormous change.”

